When To Contact A Doctor
Rashes from RA are rare and may often result from other underlying conditions. Anyone with a persistent or severe rash should find medical attention. Similarly, anyone experiencing RA symptoms, such as joint inflammation and pain, should contact a doctor.
When RA affects the skin, it can lead to serious complications. For example, rheumatoid vasculitis can cause a lack of blood flow to the extremities, which can result in poor wound healing and ulcers. Secondary infections in these wounds can cause severe complications.
People with RA may develop rashes because of other underlying conditions. Because of this, the treatment for rash symptoms will vary, depending on their cause.
For example, people with RA may experience rashes because of a reaction to or secondary hives.
Treatment for rheumatic skin conditions must be personalized for each person based on their condition and disease state. Therefore, any rash associated with RA requires a doctors supervision and treatment guidance.
What Is Rheumatoid Arthritis
Rheumatoid arthritis is a chronicsystemicinflammatoryautoimmune disease characterised by a symmetric destructive polyarthritis and extra-articularmanifestations including skin changes.
Skin changes of rheumatoid arthritis can be classified as:
- General cutaneous manifestations
- Adverse cutaneous effects of treatment.
Foamy Pink Or Brown Urine
Research suggests 30% of people with RA experience kidney problems at some point,15 though only a portion will develop chronic kidney disease. The kidneys filter blood, removing waste and excess water to create urine. When there is a problem with the kidneys, urine may look differentpossibly foamy, pink, or brown.
Kidney problems can also cause:
- Fatigue and/or insomnia
- Muscle cramping
Swelling related to kidney problems may also be less tender and painful than swelling related to an RA flare.
Kidney problems may be the result of:
- Body-wide inflammation related to RA
- Medications used to treat RA, including but not limited to methotrexate and nonsteroidal anti-inflammatory drugs , such as Aleve, Advil, and Celebrex
The most common kidney problems associated with RA include mesangial glomerulonephritis , membranous nephropathy, and secondary amyloidosis.15 Making an exact diagnosis typically requires a surgical biopsy and is not always necessary for treatment.
While kidney conditions can be serious and lead to chronic kidney disease, they may also be relatively mild or reversible with treatment. Physicians must evaluate each person individually.
Recommended treatment may include changes to medication, especially if medications are the suspected cause of kidney problems. Other first-line treatments may include taking steps to control blood pressure and making lifestyle changes, such as changing diet, exercising regularly, and quitting tobacco products.16
Recommended Reading: How To Relieve Stiffness From Arthritis
Rheumatoid Arthritis Can Cause A Range Of Skin Symptoms But Skin Problems Could Also Indicate You Have A Different Kind Of Arthritis To Begin With
Before the modern era of treating rheumatoid arthritis early with disease-modifying drugs, you could often guess that a person had RA just by looking at their skin. Long-term, severe rheumatoid arthritis damages small blood vessels throughout the body. This condition is called rheumatoid vasculitis, which shows up as bruising, pain, and sores on the skin. Another telltale sign of RA used to be rheumatoid nodules under the skin, often near affected joints.
We used to see nodules a lot, but these lumpy bumps about the consistency of a pencil eraser are getting less common with better therapy, says rheumatologist Kevin Deane, MD, PhD, associate professor of medicine at the University of Colorado School of Medicine.
While, thankfully, these skin conditions are no longer as common as they used to be, many people with RA can develop skin problems that raise questions about whether and how they might be related to their arthritis.
Also Check: Is Eating Tomatoes Bad For Arthritis
Shortness Of Breath Or Coughing And Risk Of Lymphoma
Rarely, shortness of breath or coughing is a sign of lymphoma, which is a cancer of the blood and lymph system. RA doubles the chances of getting lymphoma, raising the lifetime risk from about 2% to 4%.7Whelan P. Der Zusammenhang zwischen rheumatoider Arthritis und Krebs .& nbsp Z Rheumatol. 2006 65:497-504. doi:10.1007/s00393-006-0105-9 PMID:& nbsp 17004050,8Klein A, Polliack A, Gafter-Gvili A. Rheumatoid arthritis and lymphoma: Incidence, pathogenesis, biology, and outcome.& nbsp Hematol Oncol. 2018 36:733-739. doi:10.1002/hon.2525 PMID:& nbsp 29862535
Other signs and symptoms of lymphoma include swollen lymph nodes, weight loss, itchy skin, and/or night sweats. Swollen lymph nodes appear as lumps under the skin. Unlike rheumatoid nodules, these lumps are most likely to appear in the groin, armpit, or neck.
Also Check: What Are Symptoms Of Arthritis In Your Hands
Can Rheumatoid Arthritis Cause Skin Problems
Rheumatoidcanskin disordersproblemscauseandcanskinRArashesskin
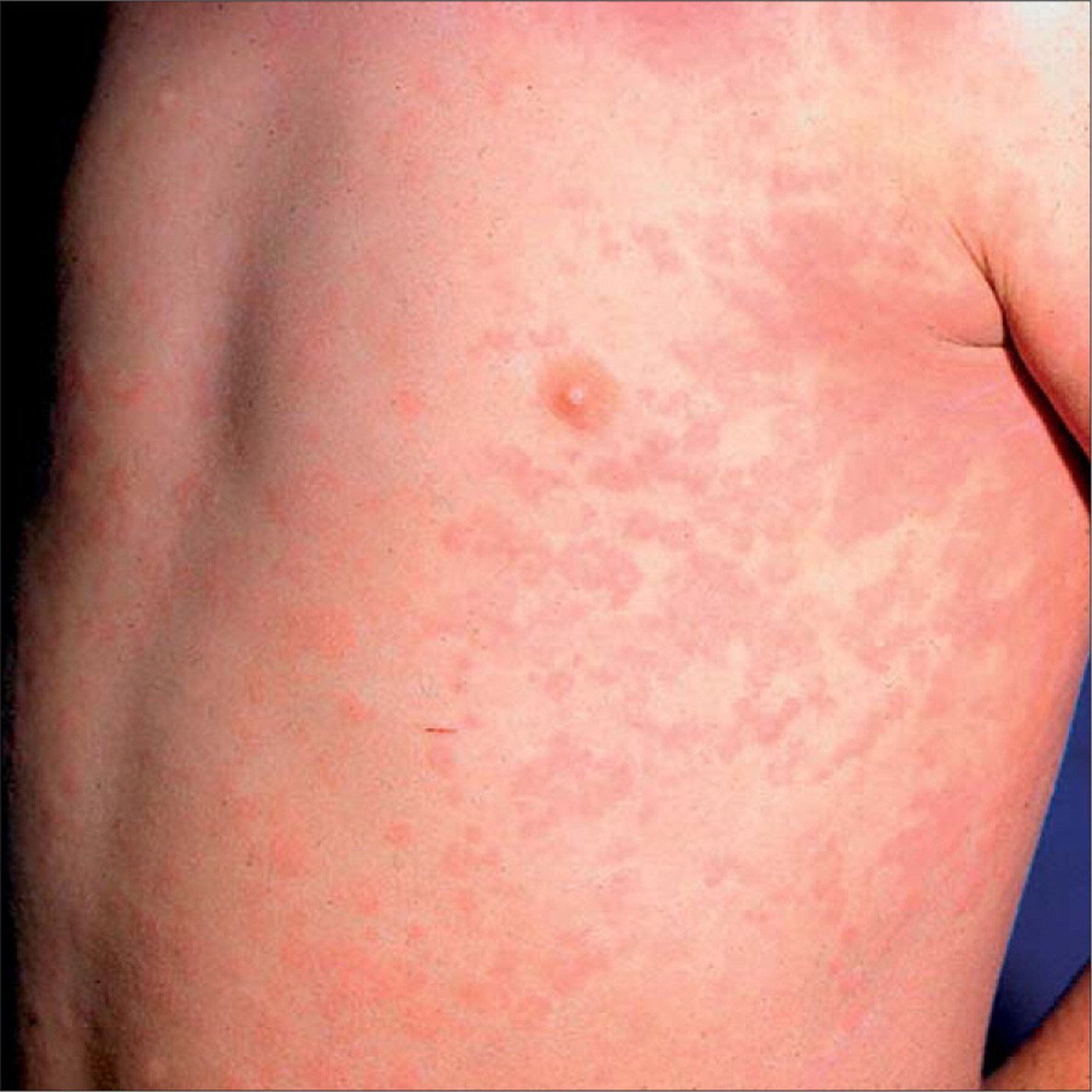
RA rashes can appear on the skin as red, painful, and itchy patches. They may also be seen as deep red pinpricks. The most common site for a rash associated with RA is on the fingertips. In some advanced cases, a rash may form painful ulcers.
Also Know, how does rheumatoid arthritis affect normal movement? Because RA damages joints over time, it causes some disability. It can cause pain and movement problems. You may be less able to do your normal daily activities and tasks. RA can also affect many non-joint parts of the body, such as the lungs, heart, skin, nerves, muscles, blood vessels, and kidneys.
Likewise, does rheumatoid arthritis cause dry skin?
Rheumatoid arthritis is frustrating enough on its own. But about 15 percent of people with RA develop a complication that affects the tear and saliva glands, causing dry mouth, dry eyes, dry skin, and additional symptoms that further aggravate their arthritis.
Is there a link between eczema and arthritis?
And eczema, psoriasis, skin infections and rosacea have also been associated with RA. Why and how RA and these skin diseases are related is a subject of research. One study found that drugs that block tumor necrosis factor one of the inflammatory proteins that are elevated in people with RA may play a role.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else.
Psoriatic arthritis can be classed as a disability if it:
- makes daily tasks difficult
- lasts for more than 12 months.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
You May Like: What Tests Are Done For Rheumatoid Arthritis
Chronic Itch Arthritis Drug Is Potential New Therapy Fighting Itch
Itching and scratching consumed Karen Bergers life until she met dermatologist Dr. Brian Kim. The itching was debilitating for two years, deeply diminishing Karens quality of life. The itching started with rashes on her back, but then it spread to most areas of her body. She described the itching as unbearable, unrelenting, uncontrollable and untreatable. It never went away.
You would scratch until you bleed. I would wake up in the morning and there would be blood on the sheets because I would scratch during the night and wasnt even aware of it, Karen said.
No one could diagnose the cause. Karen went to specialists, including dermatologists and allergists. She tried every test and cream they offered, but nothing worked. In fact, her condition got worse. Eventually, Karen was sent to see Dr. Kim.
Kim prescribed the anti-inflammatory drug Xeljanz, a rheumatoid arthritis medication. Its a potential new therapy for chronic itch. While off label for itching, Karen said she didnt have issues with insurance coverage because she has rheumatoid arthritis. It was just a matter of switching her arthritis medication to Xeljanz.
Once I started taking it, within 24 hours the intensity of the itch started to subside, said Karen. Within two to three days, it was like watching it go away. And within a week, I was fairly clear. But within two weeks, I was completely clear. I was back to my normal skin then.
Things to do in St. Louis
Donât Miss: What Causes Arthritis In Your Shoulder
Favorite Apps Products And Gadgets
CreakyJoints has partnered with rheumatology researchers at the University of Alabama at Birmingham to create this useful app that helps you track your symptoms and medications and share your experiences of living with RA. In addition to RA, the app also includes research for conditions such as ankylosing spondylitis psoriatic arthritis psoriasis osteoporosis, osteopenia, and low bone mineral density osteoarthritis fibromyalgia gout juvenile idiopathic arthritis inflammatory bowel diseases, like Crohns and ulcerative colitis lupus scleroderma polymyositis and dermatomyositis.
Dycem Super Grip Tape, $13.95
Dycem’s self-adhering Super Grip Tape provides a cushioned grip that feels more comfortable on the hands. The tape adheres to a variety of surfaces, including brooms, wheelchair arms, mobility devices, and even pens and cutlery. The nonslip grip will help increase the friction of any surface you grab.
Hamilton Beach Smooth Touch Electric Can Opener $31.85
The Smooth Touch can open both pop-top and regular cans. It is designed so that it cuts along the side of the can and not the top, minimizing the blade’s contact with food, preventing splashing, and creating a smooth, touchable lid. IMAK Compression Arthritis Gloves,$20.99
You May Like: What Doctor Deals With Arthritis
What Is A Juvenile Rheumatoid Arthritis Rash
Juvenile rheumatoid arthritis is part of a wider systemic condition known as juvenile idiopathic arthritis . This general term of arthritic conditions affects children before the age of 16 with symptoms that last for 6 weeks or longer.
One of the key symptoms can be a rash that may look pink or purple. It typically affects the trunk, arms, and legs, but not the face. It usually occurs alongside a fever.
What Is Psoriatic Arthritis Video
Psoriatic arthritis can cause pain, swelling and stiffness in and around your joints.
It usually affects people who already have the skin condition psoriasis . This causes patches of red, raised skin, with white and silvery flakes.
Sometimes people have arthritis symptoms before the psoriasis. In rare cases, people have psoriatic arthritis and never have any noticeable patches of psoriasis.
Psoriatic arthritis and psoriasis are autoimmune conditions. Our immune system protects us against illness and infection. In autoimmune conditions, the immune system becomes confused and attacks healthy parts of the body.
Both conditions can affect people of any age.
Its estimated that around one in five people with psoriasis will develop psoriatic arthritis.
People with psoriasis are as likely as anyone else to get other types of arthritis, such as osteoarthritis or rheumatoid arthritis. These conditions are not linked to psoriasis.
Psoriatic arthritis is a type of spondyloarthritis. These are a group of conditions with some similar symptoms.
Don’t Miss: Is Mango Good For Arthritis
Rheumatoid Arthritis And Skin Problems: Causes And Treatment
Rheumatoid arthritis and skin complication symptoms range from mild to severe, causing lesions. Although rheumatoid arthritis commonly affects the joints, it can involve organs and the skin, too. Many rheumatoid arthritis patients will experience skin manifestations and symptoms can vary greatly. On the severe side, skin complications can even result in lesions.
What Is A Rheumatoid Arthritis Rash
Rheumatoid arthritis is an autoimmune disease in which the bodys immune system attacks itself and inflames the protective membrane inside the joints. This can result in symptoms that range from mild to severe.
Symptoms are mostly related to joint problems. But you may also experience flare-ups in which your symptoms are worse. This may include rashes on the body due to inflammation.
Other skin conditions associated with RA can include:
- Neutrophilic dermatoses:These can include Sweets syndrome, pyoderma gangrenosum, and rheumatoid neutrophilic dermatitis.
- Urticaria:Urticaria, or hives, may occur.
- Rare skin conditions: Sometimes rare skin reactions such as erythema diutinum can occur in people with RA.
- Reactions to medications: Medications such as methotrexate can trigger rheumatoid vasculitis and periungual infarcts, or tissue death in the nails due to lack of blood supply.
In most cases, there are treatments available for RA-related rashes.
People with RA can also experience RV. RV is a rare complication experienced in only
Recommended Reading: Is Arthritis Considered Chronic Pain
What Does A Rheumatoid Arthritis Rash Look Like
One of the most common general rashes for people with rheumatoid arthritis is reddened palms, or palmar erythema. One study found that almost 60 percent of those with RA reported palmar erythema at some point. It usually occurs on both hands and is not painful or itchy. The hands may feel slightly warmer than usual.
Eczema is a common skin condition characterized by an intensely itchy, red or purple rash. While eczema can occur without rheumatoid arthritis, one study found the rates of RA in those with atopic dermatitis were 72 percent higher than in the general population. Researchers are studying whether some forms of eczema are an autoimmune disease.
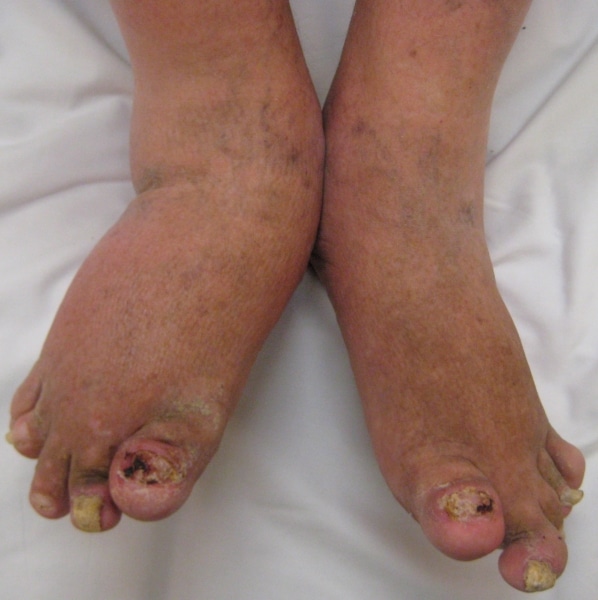
A small percentage of those with rheumatoid arthritis may develop a specific complication called cutaneous vasculitis. I had this rash on my ankles and legs when my RA flared up, but they diagnosed it as vasculitis, one myRAteam member said.
Cutaneous vasculitis is also sometimes referred to as rheumatoid vasculitis. It usually appears as a purplish rash on the skin. In more severe cases, skin ulcers may appear on the legs. The rash is often accompanied by lack of sensation, numbness, or tingling in the affected area. Other parts of the body may also experience symptoms of rheumatoid vasculitis: the liver or spleen may be enlarged, and hematuria can occur as well. Cutaneous vasculitis is an emergency, and you should talk to your rheumatologist about it right away if you notice symptoms.
Treatment Of Rheumatoid Nodules
Rheumatoid nodules are not known to be painful, so they typically are not treated aggressively. However, the nodules can become infected at the surface at that time, aggressive treatment of the infection is suggested.
Occasionally, nodules may become painful if they are in sensitive locations or are putting pressure on nerves. In this case, the nodules may be aggressively treated.
Research shows that DMARDs may reduce the size of the nodules. However, a certain DMARD, methotrexate, may increase the size of the nodules. Steroid injections can also shrink the nodule.
For nodules that cause severe pain, surgery may be indicated to remove the nodule fully.
Unfortunately, nodules that reduce or even go away due to aggressive therapy may come back RA by nature is a disease that comes and goes, so nodules may do the same.
Dont Miss: Whats Best To Take For Arthritis
Also Check: What Is Seronegative Rheumatoid Arthritis
What Causes Rheumatoid Vasculitis
According to Dr. Maya, rheumatoid vasculitis is an immune reaction that has to do with the heightened autoimmune state related to RA.
However, beyond that, experts still don’t exactly know what causes it. It’s most likely a combination of uncontrolled RA, genetic predisposition, drug reactions, and infection or virus. It’s also thought that higher levels of certain antibodies and proteins often found in the blood of people with RA may contribute to the risk.
Key Points About Psoriatic Arthritis In Children
-
Psoriatic arthritis is a rare form of arthritis or joint inflammation that affects both skin and joints. It can occur in people who have the skin disease psoriasis.
-
It is most common in adults ages 30 to 50. But it can start in childhood.
-
This condition causes inflamed, swollen, and painful joints. It also causes eye pain and fatigue.
-
Treatment may include medicines, heat and cold, splints, exercise, physical therapy, and surgery.
-
Early treatment can help the disease go into remission. Delayed treatment may lead to long-term disability.
You May Like: What Foods Should Be Avoided With Rheumatoid Arthritis
What Is The Outlook For People With Rheumatoid Arthritis Rashes
There are no permanent solutions that can completely prevent RA rashes from occurring. Doctors may try a combination of medications to help you manage your condition. These treatments may reduce inflammation and minimize joint damage.
Its important that people with RA take measures to live as healthy a lifestyle as possible. Examples of lifestyle practices that may benefit a person with RA include:
- Getting plenty of rest, which can help to reduce fatigue symptoms and minimize joint inflammation.
- Exercising whenever possible, which can help to enhance joint mobility and build strong, flexible muscles.
- Taking measures to cope with stress, such as meditation, reading, taking a walk, or doing other activities to promote relaxation.
- Eating a balanced diet full of fruits, vegetables, whole grains, and lean proteins. This can help you maintain a moderate weight, which is important in supporting joint health.
Articular Features Of Rheumatoid Arthritis
Rheumatoid arthritis initially affects the small joints, such as those in the hands, but in later stages can affect any joint. It presents as episodic flares of symmetrical synovitis , morning stiffness, and enthesitis. Untreated, it progresses to irreversible joint destruction with loss of cartilage and bone.
Also Check: What Is Inflammatory Arthritis Mayo Clinic